
Do you know the Medicare path you’ve chosen?
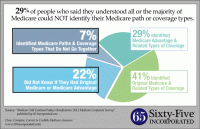 In a survey of over 800 Medicare beneficiaries, almost a quarter of those who claim to understand Medicare did not know whether they have Original Medicare or Medicare Advantage. They really don’t know Medicare at all. The first decision you must make when enrolling in Medicare is the path to take. There are two.
In a survey of over 800 Medicare beneficiaries, almost a quarter of those who claim to understand Medicare did not know whether they have Original Medicare or Medicare Advantage. They really don’t know Medicare at all. The first decision you must make when enrolling in Medicare is the path to take. There are two.
- Original Medicare (also known as Traditional Medicare) is the coverage your grandparents had. It is overseen by the Federal government and starts with Part A, hospital insurance, and Part B, medical insurance. Optional add-ons include Part D, prescription drug coverage, and a Medigap policy, Medicare supplement insurance.
- Medicare Advantage, introduced in 2003, is Medicare provided by private insurance companies approved by the Federal government. All Medicare Advantage plans must cover the same Part A and Part B services as Original Medicare. Some plans also include prescription drug coverage and are called MA-PD plans.
It’s important to know the path you’ve selected because it affects your benefits, costs, and services. Here are just three examples with the implications.
- Networks: A network is a group of healthcare providers, including physicians and hospitals, who have agreed to accept a Medicare Advantage plan’s terms. Original Medicare does not employ networks.
Implication: Original Medicare beneficiaries can see any physician anywhere in the country who participates in the Medicare program. Medicare Advantage members’ choices may be limited by the plan’s network. Most plans won’t pay for out-of-network care except in an emergency. - Out-of-pocket costs for medical services: A Medigap policy can cover many of Original Medicare’s deductibles and copayments. There is no supplemental coverage for Medicare Advantage policies. However, Medicare Advantage plans have an annual out-of-pocket spending limit.
Implication: Because there is no supplemental coverage, those with Medicare Advantage members must cover deductibles and copayments for physician visits and hospital stays, to name just two. For example, one plan charges $450 a day for the first six days of a hospital stay. A plan member could be responsible for up to $6,500, the plan's limit.
The costs for a Medicare Advantage plan member who is hospitalized frequently could hit the spending limit and then there would no additional out-of-pocket costs for covered services for the remainder of the year. There is no limit on spending for Original Medicare beneficiaries; however, a Medigap policy can lessen the sting. - Premiums: Premiums for a Medicare Advantage plan tend to lower. There are zero-premium plans available to most beneficiaries in the country. Medigap policies have monthly premiums, which can increase over the year.
Implication: The choice depends on how a person wants to handle out-of-pocket costs. - Optional benefits: Both Original Medicare and Medicare Advantage cover services for the treatment of medical conditions and some preventive care. However, Medicare Advantage plans have the freedom to include other benefits, such as dental and vision care.
Implication: Original Medicare does not cover any of the optional services offered by many Medicare Advantage plans. Granted those services won’t be free for plan members but the plans can help cut the out-of-pocket costs.
What should you do? Find out what type of coverage you have. Start with the insurance cards in your wallet. If you see the word, “Supplement,” you chose Original Medicare with a Medigap policy. If your card identifies a plan that has drug coverage, you porbably went the route of Medicare Advantage. If you’re not sure, call the number on the card and ask, “Is this plan Medicare Advantage or a supplement?” Then you’ll know your coverage.
Last updated: 02-27-2024
